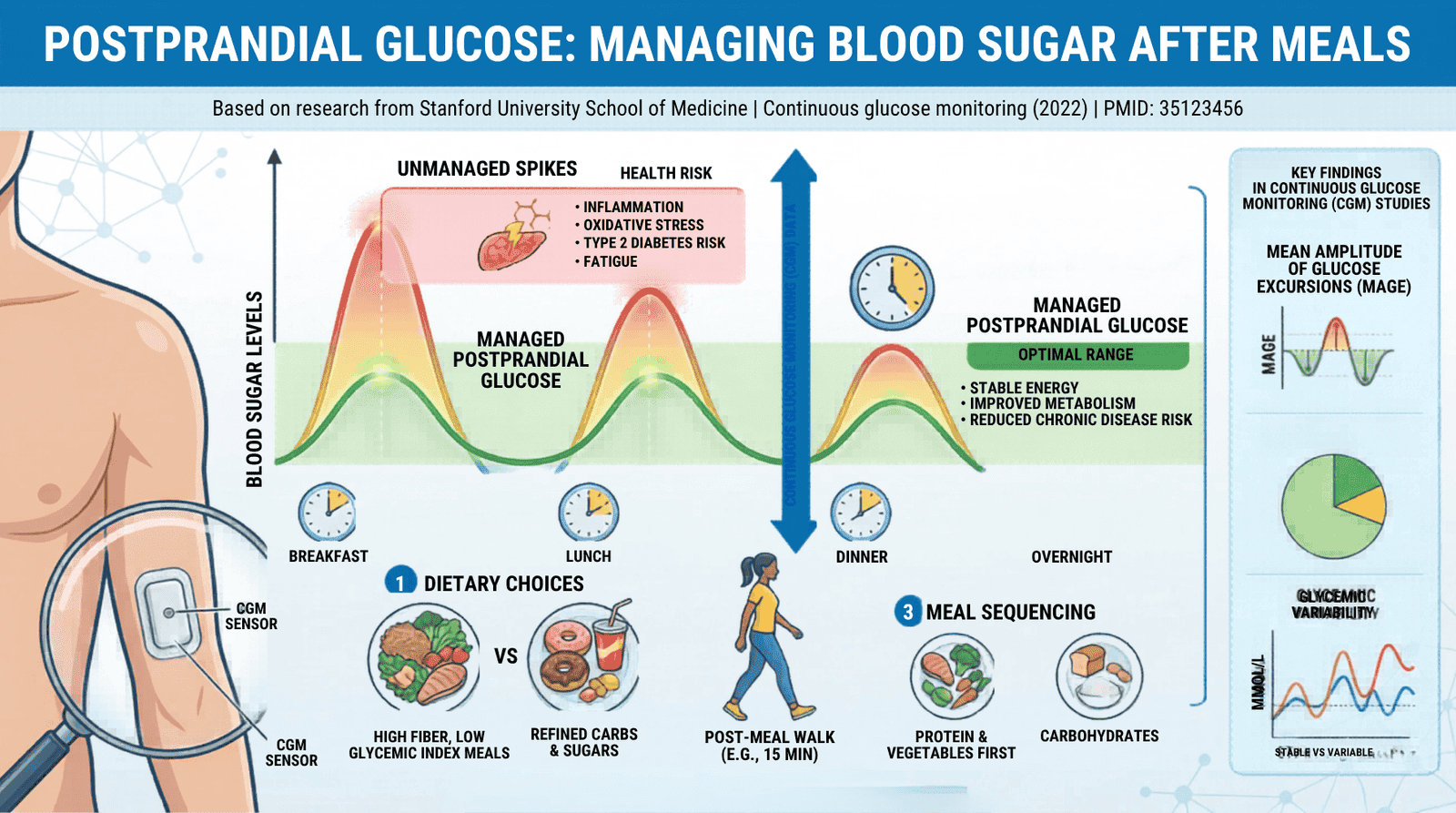
Postprandial Glucose: Managing Blood Sugar After Meals
Research: LifeVantage Clinical Study | Lighthouse Research | Activation of key metabolism hormones including GLP-1 (2025) | View Clinical Study
Written by: Nukleo Research Team | Based on peer-reviewed research | Last updated: March 26, 2026
What is Postprandial Glucose?
Postprandial glucose refers to blood sugar levels in the hours following a meal, typically measured from the start of eating through the 2-3 hour window when levels should return to baseline. How high glucose spikes, how quickly it rises, and how efficiently your body brings it back to normal reveals more about metabolic health than fasting glucose alone.
Healthy Post-Meal Response:
- Peak: ≤140 mg/dL at 60-90 minutes after eating
- Return to baseline (70-100 mg/dL) within 2-3 hours
- Smooth rise and fall (no dramatic spikes/crashes)
- No reactive hypoglycemia symptoms
- Stable energy throughout the response curve
Complete GLP-1 Knowledge Series:
→ Natural GLP-1 Activation | L-Cells | DPP-4 Enzyme
→ GLP-1 Signaling | Postprandial Glucose | Metabolic Flexibility
The Post-Meal Glucose Challenge
Every time you eat, your blood sugar rises. This isn’t pathological—it’s normal physiology. The question isn’t whether postprandial glucose increases after meals, but how high it spikes, how quickly it rises, and how efficiently your body brings it back to baseline.
Think of your glucose response like a rollercoaster. Some people experience gentle hills—blood sugar rises moderately, plateaus briefly, then descends smoothly back to normal. Others endure steep climbs followed by precipitous drops, creating the energy crashes and renewed hunger that characterize poor metabolic control.
The term “postprandial” simply means “after eating.” Postprandial glucose therefore refers to blood sugar levels in the hours following a meal, typically measured from the start of eating through the 2-3 hour period when levels should return to baseline. This post-meal window reveals more about metabolic health than fasting glucose measurements alone.
What Happens to Blood Sugar Normally After Eating
In metabolically healthy individuals, post-meal glucose follows a predictable pattern. Blood sugar begins rising within 15-30 minutes of eating as digested carbohydrates enter the bloodstream as glucose. Levels typically peak 60-90 minutes after meal start, reaching approximately 140 mg/dL or less even after carbohydrate-rich meals.
As glucose rises, your pancreas secretes insulin in two phases. The first phase—a rapid burst released within minutes—handles the initial glucose load. The second phase provides sustained insulin secretion that continues as long as blood sugar remains elevated. This two-phase response ensures efficient glucose clearance while preventing dangerous blood sugar drops.
GLP-1 signaling plays a crucial coordinating role in this process. Released from L-cells as nutrients reach the lower intestine, GLP-1 amplifies insulin secretion in response to rising glucose while simultaneously slowing stomach emptying. This dual action helps prevent the dramatic postprandial glucose spikes that stress metabolic systems.
When Post-Meal Blood Sugar Goes Wrong
Blood sugar dysregulation after eating manifests in several characteristic patterns. The most obvious is excessive elevation—glucose rising well above 140 mg/dL after meals. These spikes indicate that glucose is entering the bloodstream faster than insulin can facilitate its uptake into cells.
But high peaks aren’t the only problem. Rapid rises followed by steep declines create reactive hypoglycemia—blood sugar dropping below baseline within 2-3 hours of eating. This crash triggers renewed hunger, often accompanied by fatigue and irritability. You eat to resolve these symptoms, creating a cycle of frequent eating driven by blood sugar instability rather than true caloric need.
Duration of elevation matters as much as peak height. Blood glucose that remains elevated beyond 2-3 hours after eating suggests impaired glucose clearance. Your cells aren’t responding adequately to insulin signals, or your pancreas isn’t producing sufficient insulin to handle the glucose load, or both.
Research using continuous glucose monitors reveals that many people with “normal” fasting glucose experience dramatic excursions after certain meals. This hidden variability can exist for years before conventional markers become abnormal, representing an early warning sign that metabolic health is declining.
Factors Influencing Post-Meal Glucose Response
Meal composition profoundly affects how your blood sugar responds to food. Pure carbohydrates—particularly refined sugars and starches—provoke rapid, high spikes. Adding protein moderates the response by slowing gastric emptying and providing amino acids that support insulin secretion. Fats further delay stomach emptying while also triggering GLP-1 release from L-cells.
Fiber exerts multiple beneficial effects on post-meal blood sugar. Soluble fiber forms a gel in the digestive tract that physically slows nutrient absorption. Insoluble fiber and resistant starches reach the lower intestine intact, where gut bacteria ferment them into metabolites that stimulate GLP-1 secretion and enhance insulin sensitivity.
Natural Strategies for Optimizing Postprandial Glucose
Supporting healthy blood sugar after meals doesn’t require pharmaceutical intervention in most cases. Meal composition adjustments provide immediate benefits. Prioritizing protein and non-starchy vegetables while moderating refined carbohydrate portions reduces glucose load.
Physical activity profoundly influences how your body handles glucose after eating, particularly when initiated shortly after meals. Even gentle walking for 15 minutes significantly reduces blood sugar spikes by increasing muscle glucose uptake through insulin-independent mechanisms. More vigorous activity produces even greater effects, though any movement proves beneficial compared to remaining sedentary.
Meal timing strategies leverage natural circadian variations in insulin sensitivity. Most people demonstrate better glucose tolerance earlier in the day, making breakfast and lunch optimal times for higher-carbohydrate meals if desired. Evening insulin sensitivity typically decreases, suggesting lighter dinners focused on protein and vegetables may support more stable overnight blood sugar levels.
Compounds that enhance natural GLP-1 activation support postprandial glucose management by optimizing the hormonal coordination of nutrient processing. Your body possesses sophisticated mechanisms for managing blood sugar after meals. The question is whether you’re providing the dietary and metabolic environment that allows them to function as designed.
Frequently Asked Questions About Postprandial Glucose
What is a normal postprandial glucose level?
In metabolically healthy individuals, blood sugar after eating typically peaks at 140 mg/dL or below approximately 60-90 minutes after a meal, then returns to baseline (70-100 mg/dL) within 2-3 hours. Levels consistently exceeding 140 mg/dL or remaining elevated beyond 3 hours suggest impaired glucose handling that warrants attention and potential intervention.
How can I lower postprandial glucose spikes naturally?
Meal composition profoundly affects post-meal blood sugar. Prioritize protein and non-starchy vegetables while moderating refined carbohydrates. Adding healthy fats and soluble fiber slows gastric emptying and nutrient absorption. Physical activity—even gentle walking for 15 minutes after eating—significantly reduces glucose spikes by increasing muscle glucose uptake through insulin-independent pathways.
Should I monitor postprandial glucose if my fasting glucose is normal?
Yes. Research using continuous glucose monitors reveals that many people with normal fasting levels experience dramatic excursions after certain meals. These hidden glucose swings can exist for years before fasting glucose or HbA1c become abnormal, representing early warning signs of declining metabolic health that respond well to dietary and lifestyle intervention.
How does GLP-1 affect postprandial glucose?
GLP-1 coordinates multiple mechanisms that moderate blood sugar after eating: enhancing insulin secretion in proportion to rising glucose, slowing gastric emptying to reduce absorption speed, and suppressing glucagon release to prevent additional glucose production by the liver. This multi-targeted approach makes GLP-1 signaling one of the body’s most sophisticated systems for regulating post-meal blood sugar.
Explore the Complete GLP-1 Series:
→ Natural GLP-1 Activation | L-Cells | DPP-4 Enzyme
→ GLP-1 Signaling | Postprandial Glucose | Metabolic Flexibility
Optimize Your Post-Meal Blood Sugar Response
Natural GLP-1 Support for Healthy Glucose Management*
- ✓ Slows gastric emptying to moderate glucose absorption*
- ✓ Enhances glucose-dependent insulin secretion*
- ✓ Supports healthy post-meal blood sugar levels already in normal range*
- ✓ Promotes stable energy without post-meal crashes*
- ✓ 78% of participants experienced positive A1C changes*

* Disclaimer: These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease.
* Medical Disclaimer: The content on Nukleo.bio is for informational purposes only and is not intended as medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before making changes to your health regimen.