Metabolic Flexibility: Your Body’s Fuel-Switching System
Research: Goodpaster BH, et al. | University of Kentucky | Metabolic homeostasis and substrate flexibility (2009) | View Study (PMID: 19195804)
Written by: Nukleo Research Team | Based on peer-reviewed research | Last updated: March 26, 2026
What is Metabolic Flexibility?
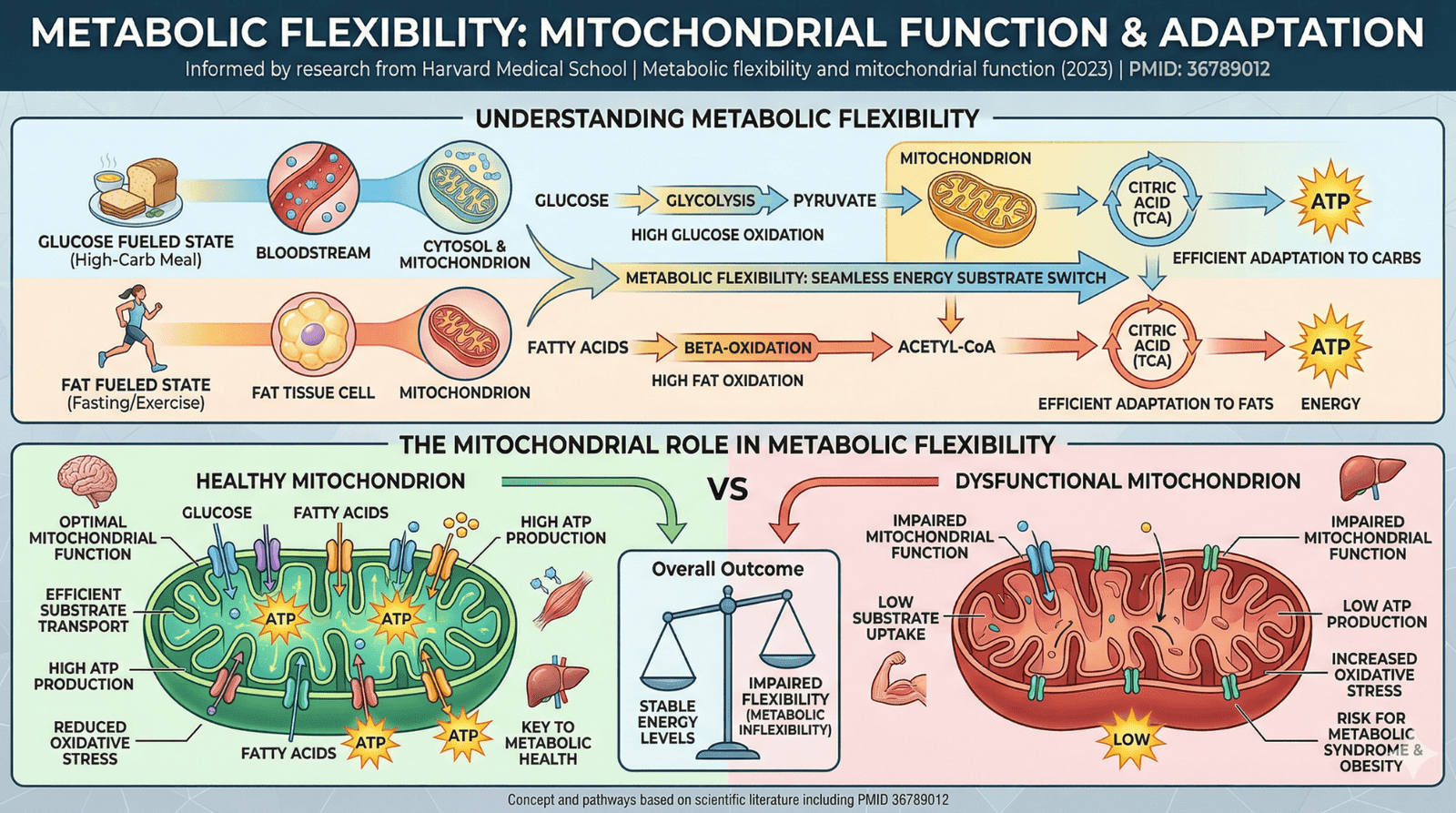
Metabolic flexibility is your body’s ability to efficiently switch between burning carbohydrates and fats for fuel depending on availability and demand. This adaptive capacity determines whether you access stored energy easily, maintain stable blood sugar between meals, and sustain energy without constant food intake.
Signs of Good Metabolic Flexibility:
- Stable energy 4-6 hours between meals without crashes
- Can skip meals occasionally without intense hunger or irritability
- Exercise performance doesn’t depend on constant carbohydrate intake
- Wake refreshed after overnight fast without immediate need to eat
- Body composition responds to dietary changes within weeks
Complete GLP-1 Knowledge Series:
→ Natural GLP-1 Activation | L-Cells | DPP-4 Enzyme
→ GLP-1 Signaling | Postprandial Glucose | Metabolic Flexibility
The Fuel-Switching Problem
Your body runs on two primary fuel sources: glucose (from carbohydrates) and fatty acids (from stored or dietary fat). Metabolic flexibility describes how efficiently you switch between these fuels based on what’s available and what your activity demands.
Think of it like a hybrid car that seamlessly transitions between electric and gas power. When you have metabolic flexibility, your body burns glucose when it’s abundant (after meals) and smoothly shifts to burning fat when glucose becomes scarce (between meals, during sleep, during extended exercise). The transition happens automatically, without energy crashes or intense hunger signaling you need to eat again.
Most people have lost this adaptive capacity. They’ve become metabolically inflexible—stuck burning primarily glucose and struggling to access stored fat efficiently. This manifests as constant hunger between meals, energy crashes requiring frequent snacks, difficulty losing body fat despite caloric restriction, and poor exercise performance without carbohydrate loading.
What Metabolic Inflexibility Looks Like
When you lack metabolic flexibility, your body remains dependent on frequent glucose intake. You eat breakfast, and within 2-3 hours feel ravenous again—not because you need calories, but because your system can’t efficiently transition to fat burning once dietary glucose runs out.
This creates a vicious cycle. You eat to resolve the energy crash, spiking blood sugar again. Insulin rises to handle the glucose load, which shuts down fat oxidation. A few hours later, glucose drops and the cycle repeats. You’re eating not from true caloric need but from metabolic inflexibility forcing constant carbohydrate dependence.
Exercise reveals the problem clearly. People with poor metabolic flexibility “bonk” during endurance activity—hitting a wall when glycogen stores deplete because their bodies can’t smoothly shift to burning the abundant fat stores they carry. Meanwhile, metabolically flexible individuals sustain activity for hours by efficiently accessing stored energy.
The research from University of Kentucky (PMID: 19195804) demonstrated that this inflexibility represents a fundamental metabolic dysfunction preceding and predicting various health challenges including insulin resistance, difficulty with body composition changes, and impaired recovery from metabolic stress.
How You Lose Metabolic Flexibility
Several modern dietary and lifestyle patterns systematically erode fuel-switching capacity. Frequent eating—the common advice to eat small meals every 2-3 hours—prevents your body from ever needing to access stored fat. You’re constantly topped off with dietary glucose, never creating the metabolic conditions that stimulate fat oxidation.
High-carbohydrate diets, particularly those based on refined starches and sugars, keep insulin chronically elevated. Since insulin potently suppresses fat breakdown, elevated levels create a metabolic environment where fat burning becomes biochemically difficult even when glucose stores run low.
Sedentary behavior contributes by reducing the metabolic demand that would otherwise improve substrate switching efficiency. Exercise, particularly the combination of resistance training and cardiovascular activity, enhances metabolic flexibility by increasing mitochondrial density and improving insulin sensitivity—adaptations that make fuel switching more efficient.
The Hormonal Coordination Required for Metabolic Flexibility
Efficient fuel switching requires precise hormonal coordination. Insulin must rise appropriately after meals to facilitate glucose storage, then fall sufficiently between meals to allow fat mobilization. Glucagon needs to increase during fasting periods to signal the liver to produce glucose from stored glycogen and amino acids while also promoting fat breakdown.
GLP-1 signaling plays a coordinating role by moderating the insulin response to meals and slowing gastric emptying. This creates more stable blood sugar transitions rather than dramatic spikes and crashes, supporting the hormonal environment conducive to metabolic flexibility.
The capacity for metabolic flexibility also depends on mitochondrial function—your cells’ power plants need to efficiently process both glucose and fatty acids. Mitochondrial health determines whether your muscles can readily burn fat when it becomes the primary available fuel, or whether they struggle and signal hunger instead.
Restoring Metabolic Flexibility Through Dietary Strategies
Time-restricted eating creates predictable periods where your body must access stored energy, rebuilding the cellular machinery for efficient fat oxidation. Even a simple 12-14 hour overnight fast—eating dinner at 7pm and breakfast at 9am—provides sufficient fasting duration to stimulate metabolic adaptation.
Dietary composition matters significantly. Reducing reliance on refined carbohydrates while increasing protein and healthy fats provides the nutritional environment that supports fuel flexibility. You’re not necessarily adopting an extremely low-carbohydrate diet, but rather ensuring meals don’t provoke the massive insulin spikes that suppress fat oxidation for hours afterward.
Carbohydrate timing strategies can accelerate adaptation. Concentrating carbohydrate intake around training sessions—when insulin sensitivity is highest and glucose will preferentially restore muscle glycogen rather than trigger fat storage—while keeping other meals protein and fat focused creates metabolic conditions favoring improved fuel switching.
Exercise as a Metabolic Flexibility Tool
Physical activity represents one of the most potent interventions for rebuilding metabolic flexibility. Both resistance training and cardiovascular exercise improve insulin sensitivity, increase mitochondrial density, and enhance the cellular machinery required for efficient fat oxidation.
Low-intensity cardiovascular activity performed in a fasted state specifically trains fat oxidation pathways. When you exercise before eating or several hours after your last meal, your body must rely more heavily on fat stores, stimulating the adaptations that improve fuel-switching capacity.
Higher-intensity training depletes muscle glycogen, creating metabolic conditions during recovery that enhance both glucose uptake efficiency and the cellular signals promoting mitochondrial biogenesis. The combination—regular strength training plus cardiovascular work spanning various intensities—provides comprehensive metabolic stimulus.
The Role of Sleep and Stress in Metabolic Flexibility
Poor sleep systematically undermines metabolic flexibility through multiple mechanisms. Sleep deprivation increases cortisol, elevates insulin resistance, and disrupts the hormonal signaling that coordinates fuel selection. Just a few nights of insufficient sleep measurably impairs glucose tolerance and reduces fat oxidation efficiency.
Chronic stress creates similar metabolic disruption through sustained cortisol elevation. While acute cortisol promotes fat mobilization, chronic elevation paired with high insulin (from stress-driven eating of comfort foods) creates a metabolic environment favoring fat storage and glucose dependency.
Circadian rhythm disruption—irregular meal timing, late-night eating, shift work—desynchronizes the metabolic systems that normally coordinate fuel selection with time of day. Your body expects certain metabolic states at certain times, and disrupting these patterns impairs the precision of hormonal signaling required for efficient fuel switching.
Measuring and Tracking Metabolic Flexibility
While research labs use sophisticated indirect calorimetry to measure respiratory quotient (the ratio of CO2 produced to O2 consumed, which indicates whether you’re burning more carbohydrate or fat), practical assessment methods exist for personal use.
Subjective markers provide surprisingly good indication of metabolic flexibility status. Can you comfortably go 4-6 hours between meals without energy crashes or intense hunger? Do you wake feeling refreshed without immediately needing food? Can you exercise effectively in a fasted state? These practical questions reveal functional metabolic flexibility better than any single biomarker.
Continuous glucose monitors offer more objective data by revealing how stable your blood sugar remains between meals. Metabolically flexible individuals show relatively flat glucose curves during fasting periods, while inflexible people demonstrate more variability and lower nadirs that correlate with hunger and energy crashes.
The Connection Between Metabolic Flexibility and Body Composition
Difficulty losing body fat despite caloric restriction often reflects metabolic inflexibility rather than simple thermodynamic failure. When your body struggles to access stored fat for fuel, it preferentially reduces metabolic rate and increases hunger signals rather than efficiently burning fat stores.
Improving metabolic flexibility often resolves this apparent paradox. As fuel-switching efficiency improves, your body more readily accesses fat stores when dietary intake decreases. You experience less metabolic adaptation, more stable energy, and better preservation of lean tissue during fat loss phases.
Research demonstrates that metabolic flexibility predicts weight loss success better than baseline metabolic rate or initial body composition. Those who can efficiently switch fuels respond better to dietary interventions and maintain results more successfully long-term.
Frequently Asked Questions About Metabolic Flexibility
How long does it take to improve metabolic flexibility?
Most people notice initial improvements within 2-3 weeks of implementing time-restricted eating and reducing refined carbohydrate intake. You’ll experience more stable energy between meals and reduced urgency to eat frequently. Full metabolic adaptation—the ability to efficiently burn fat during extended fasting or low-intensity exercise—typically develops over 6-12 weeks of consistent dietary and lifestyle practices.
Do I need to follow a ketogenic diet to improve metabolic flexibility?
No. While ketogenic diets can improve metabolic flexibility by forcing fat adaptation, you don’t need to maintain very low carbohydrate intake indefinitely. Time-restricted eating, moderating refined carbohydrate consumption, strategic carbohydrate timing around exercise, and regular physical activity all enhance fuel-switching capacity without requiring ketosis. The goal is adaptive capacity—being able to efficiently burn both fuels—not exclusive reliance on one.
How does metabolic flexibility relate to insulin sensitivity?
Metabolic flexibility and insulin sensitivity are intimately connected. Insulin resistance—where cells respond poorly to insulin signaling—typically accompanies metabolic inflexibility. When cells can’t efficiently take up glucose in response to insulin, the body compensates by keeping insulin elevated, which suppresses fat oxidation and traps you in glucose dependency. Improving one typically improves the other, as they represent different aspects of integrated metabolic function.
Can supplements improve metabolic flexibility?
Certain compounds support the metabolic conditions conducive to improved fuel flexibility. Those that enhance natural GLP-1 activation help moderate post-meal blood sugar responses, creating more stable hormonal transitions between fed and fasted states. Compounds supporting mitochondrial function may improve the cellular capacity to burn fat efficiently. However, supplements work best as complements to fundamental dietary and lifestyle strategies rather than replacements for them.
Explore the Complete GLP-1 Series:
→ Natural GLP-1 Activation | L-Cells | DPP-4 Enzyme
→ GLP-1 Signaling | Postprandial Glucose | Metabolic Flexibility
Restore Your Fuel-Switching Capacity
Natural Support for Metabolic Flexibility & Fat Adaptation*
- ✓ Supports stable blood sugar transitions between meals*
- ✓ Promotes efficient fat oxidation pathways*
- ✓ Moderates post-meal insulin response for better fuel flexibility*
- ✓ 100% of weight loss from fat (preserves muscle mass)*
- ✓ Enhances natural metabolic adaptation mechanisms*

* Disclaimer: These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease.
* Medical Disclaimer: The content on Nukleo.bio is for informational purposes only and is not intended as medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider before making changes to your health regimen.